Loss Of Smell (Anosmia)
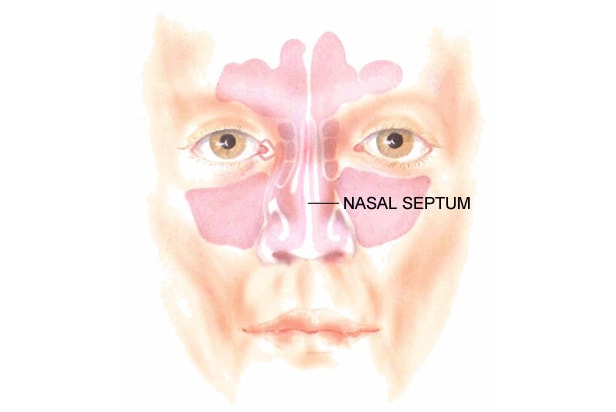
The three most common causes for a smell disorder are sinonasal disease, after a viral URTI and after a head or facial injury when shearing of the olfactory fibres near the cribriform plate may occur. As the olfactory receptors are at the very top of the nose any condition blocking the passage of air to this area can reduce the sense of smell, such as nasal polyps.
Diagnostics
Nasal Rigid / Flexible Endoscopy for a detailed assessment of the inside of the nose. Skin Prick Allergy Test and RAST Allergy Test if possible rhinitis symptoms are present.
Nasal Rigid / Flexible Endoscopy
Why?
The nostrils are quite small, so even using a very bright halogen headlight and a dilator instrument (speculum) to expand the nostril, it is impossible to see any more than the front part inside the nasal cavity. The introduction of a small sterile rigid endoscope with an angled lens, or a sterile flexible endoscope whose tip can be manually rotated in various directions, allows a very detailed inspection of the whole of the nasal cavity and the site of the sinus openings. Further back the nasopharynx and Eustachian tube openings can also be examined.
How?
Cophenylcaine, a surface local anaesthetic and decongestant, is sprayed into each nostril held open by a dilator speculum. This drug is absorbed very quickly and numbs and shrinks the nasal lining. Although the introduction of an endoscope is an unusual feeling it is not unpleasant. The subsequent examination will take less than 5 minutes.

Nasal Fluid For Beta 2 Transferrin Assay
Why?
The top of the nose and several of the sinuses (frontal, ethmoid and sphenoid) are adjacent to parts of the brain cavity. Defects in the brain covering (dura) may result in the escape of brain fluid (CSF) into the sinuses and/or nasal cavity. The liquid is transparent and very thin like water, but can still be difficult to distinguish from clear profuse watery serous nasal secretions. Untreated CSF rhinorrhoea may result in the serious complication of meningitis, so early surgery to repair any defect is essential.
How?
Brain fluid will always drip from the front of the nose when the person leans forwards. A couple of drops of this nasal fluid is collected in a sterile container and stored in a refrigerator. This is a very specialised test which is only undertaken in very few laboratories. Our samples are sent to the Department of Neuro-immunology at The National Hospital, Queen Square, where one of our Clinic team collaborated with this unit 20 years ago to develop this important diagnostic tool.
Skin Prick Allergy Test
Why?
Allergies are common and it is thought that about 1 in 3 of the population will consult a doctor at some time in their life with allergic symptoms. Many cases of rhinitis (tissue inflammation that causes persistent nasal congestion, nose bleeds, nasal itching and sneezing) can be caused by allergies.
How?
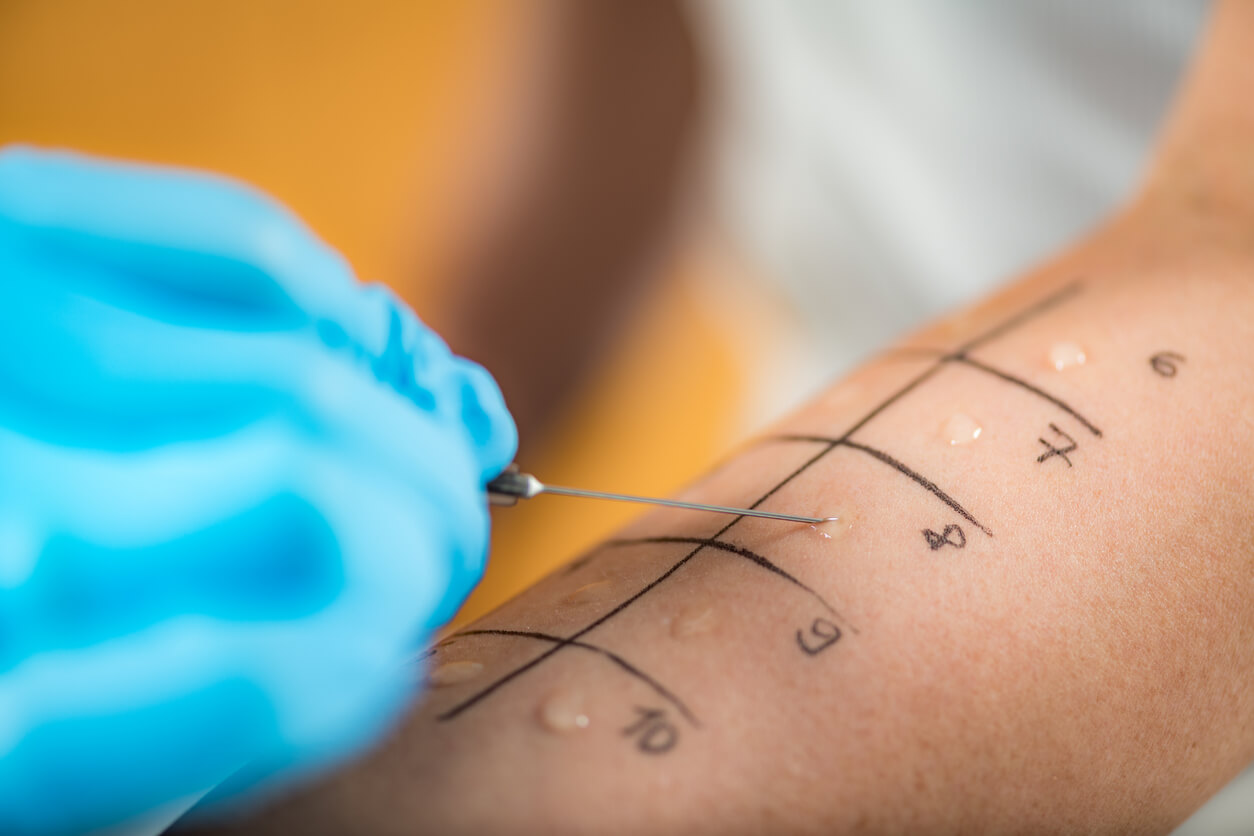
This test is simple and quick, giving results within 15-20 minutes, and is carried out by the ENT practice nurse. It is important that you do not take any form of antihistamine or steroid drug for at least 48 hours before the test as these medicines may affect the results. Allergens are introduced into the skin, usually the forearm, in such tiny amounts that testing is quite safe and can be carried out on all age groups, including babies. If you have bad eczema the test can be performed on your back.
The area to be tested is coded with a marker pen for each allergen and a drop of the solution is placed by each code. A standard concentration histamine solution is also applied to serve as a control. The skin is then pricked through the drop using the tip of a single-use sterile lancet. This can feel a little uncomfortable but should not be painful. The nurse will assess the test sites for the presence and size of redness (known as erythema) and lumps (known as wheals) after 15 minutes. The responses are compared to the control histamine solution which should always cause a reaction. The degree of reaction relative to the control indicates whether a certain level of antibodies are present which may be causing your symptoms. The wheals, which feel very much like a reaction to a nettle sting, clear within an hour for most people and any irritation can helped by applying anti-inflammatory steroid cream.

RAST Allergy Blood Test
Why?
An allergic person’s immune system produces a special type of antibody, Immunoglobulin E (IgE), to combat each specific substance to which they have an abnormal sensitivity. The RAST stands for radioallergosorbent test, which is a laboratory measure of the amount of specific IgE antibodies present in the blood.
How?
Samples of your blood are drawn from your arm at the ENT Clinic and are sent to our laboratory for analysis. The results take a few days to process but will confirm whether or not your body reacts to any substances we have tested and will also be graded to indicate the severity of the reaction. These grades range from 0-6, with 0 i
CT Scan
Why?
Computed tomography (CT) is a medical imaging method using X-ray tomography created by computer processing. It provides important diagnostic information in various anatomical planes. Conventional sinus X-rays are not really helpful, as various anatomical structures superimposed on one another prevents proper assessment of the ethmoid sinuses and ostiomeatal complex regions.
The main advantage of CT over MRI scanning is that it demonstrates bone as well as soft tissue features, and is therefore the radiological assessment of choice in patients with sinus problems
How?
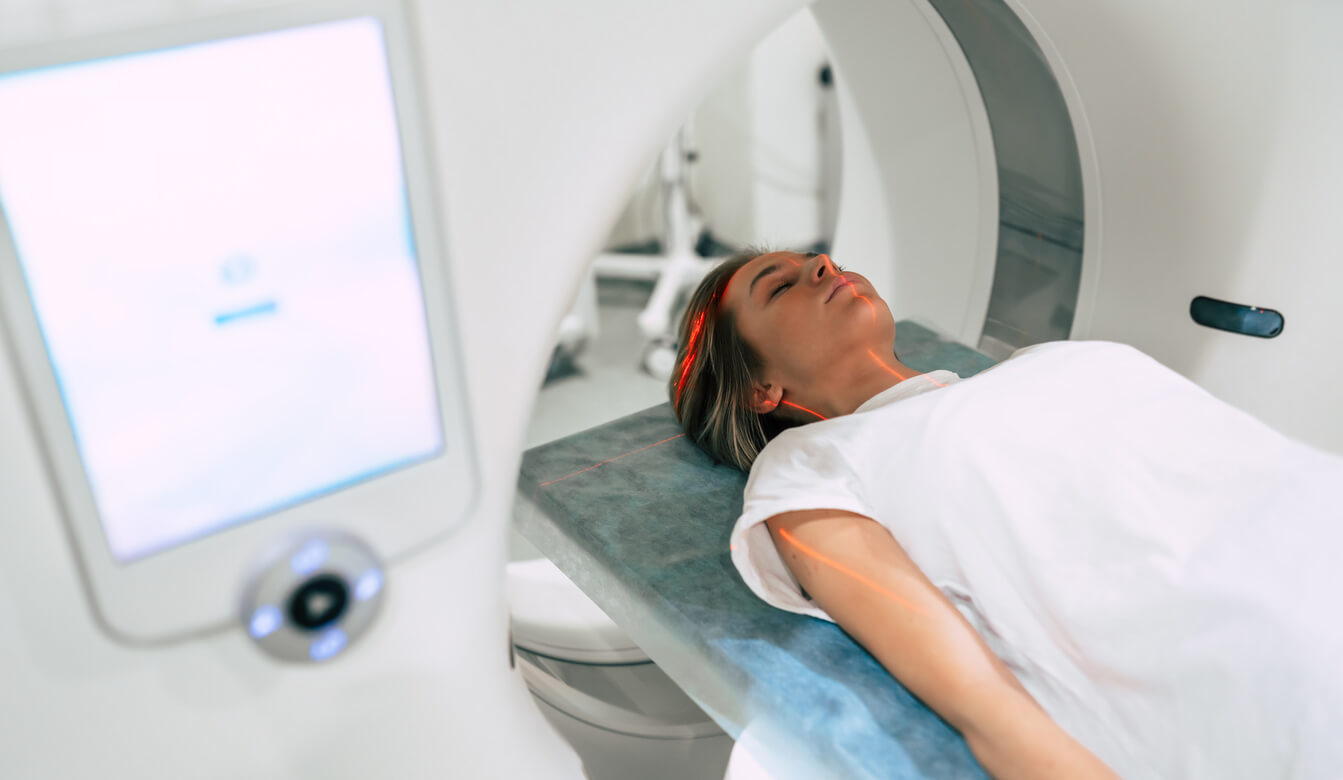
The scanning techniques involves lying still with the head in a medical “hair-dryer” open capsule for approximately 20 minutes. It is a completely painless procedure.
MRI Scan
Why?
Magnetic resonance imaging (MRI) is a medical imaging technique used in radiology to study internal soft tissue structures in detail. It provides good contrast between the different types of tissue, which is a major advantage over CT. MRI does not use ionising radiation unlike CT or traditional X-rays. Instead it uses a powerful magnetic field to align tissue atoms, and then uses radiofrequency fields to change and record their alignment. This scanned information is then used to construct images of specific parts of the body. The commonest indication for an MRI scan with nasal and sinus problems is to investigate patients with tumours or skull base disorders in more detail.
How?
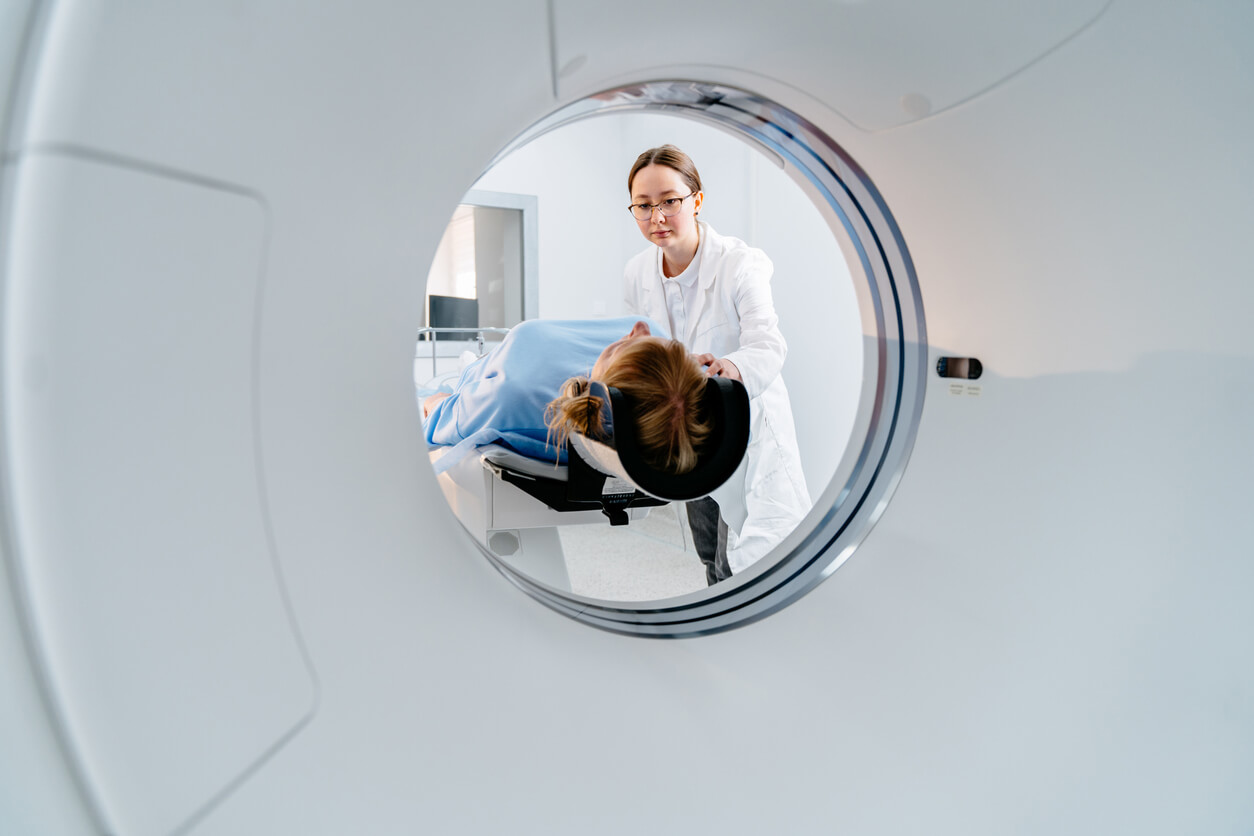
The patient lies still on a couch with their head in a metal tube for about 30 minutes. Some patients find this enclosed experience unpleasant, which has resulted in the development of so-called “open scanners”.
The private health insurances we work with
Harley Street ENT is recognised by a wide range of leading UK and international private health insurers, ensuring easy access to our care for patients with approved cover.

Need help and advice? Speak to an advisor
To discuss your needs in confidence or arrange a consultation, please contact our advisory team, who will be happy to assist you.







